Gastro-oesophageal reflux disease (GERD) is a chronic, recurring condition that can significantly impact quality of life and carries an increased risk of causing oesophageal cancer. Endoscopic pyloric tightening is now considered a safe, efficient and highly effective treatment solution for gastro-oesophageal reflux disease.
Tightening the Cardiac Sphincter to Prevent Reflux and Reduce the Risk of Oesophageal Cancer Caused from Barrett’s Oesophagus Using the Argon Plasma Ablation Technique
For many years, Mr N.H.P., a 60-year-old from Ho Chi Minh City, suffered with persistent gastro-oesophageal reflux disease (GERD). Initially, he experienced heartburn after meals, but gradually, the burning sensation in his chest became more frequent. On numerous nights, Mr P. had to sleep sitting up, as lying down would cause his stomach acid to rise into his throat. Despite seeking treatment at several hospitals, his condition remained unchanged. Over the past two years, his symptoms worsened, and he began to feel like something was stuck in his throat while eating, making it difficult for him to eat comfortably. The ongoing struggle with GERD left him feeling hopeless.
One day, when Mr P.’s wife went for a routine health check-up at FV Hospital, she learned that there was an effective treatment for GERD there. Feeling hopeful, she scheduled a consultation for Mr P. at the hospital.
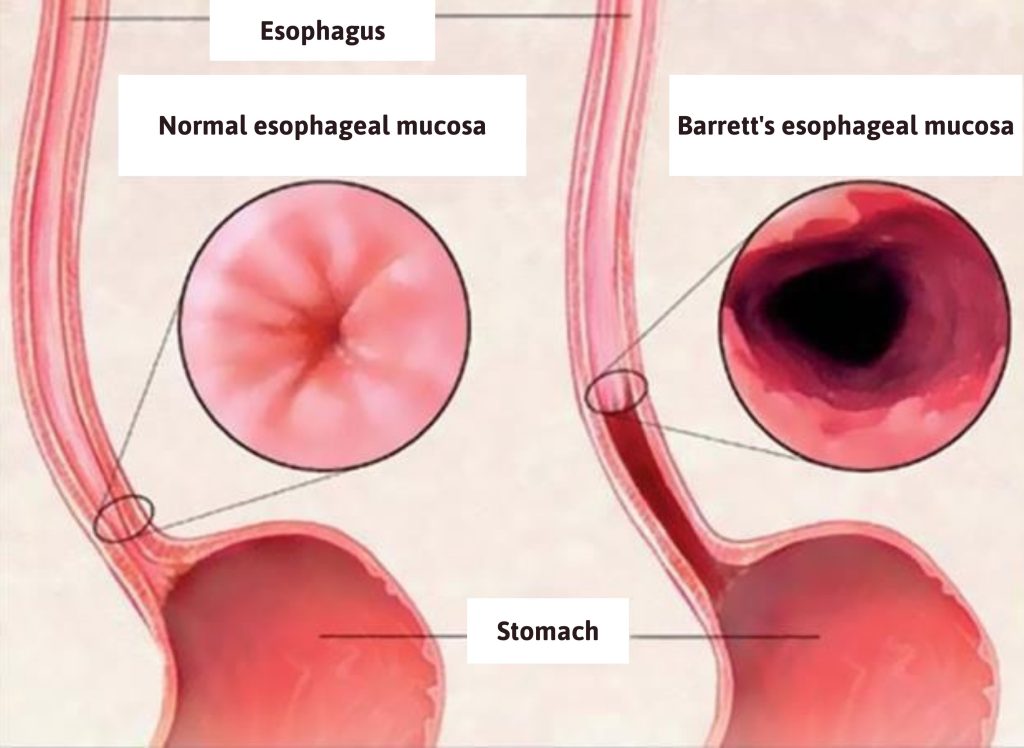
After examining Mr P. and performing an endoscopy, Dr Ngo Van Huy, Deputy Head of Gastroenterology & Hepatology Department at FV Hospital, confirmed that the patient had GERD with a grade 3-4 defect of the cardiac sphincter. More concerning, he had also developed Barrett’s oesophagus due to years of reflux – a pre-cancerous condition of the oesophagus.
Given this clinical situation, Dr Huy recommended a two-step treatment for Mr P. The first step involved controlling the reflux with an endoscopic procedure to tighten the cardiac sphincter. This would be followed by the Argon Plasma Coagulation (APC) technique, also known as Argon Plasma Ablation, to eliminate Barrett’s cells and reduce the risk of oesophageal cancer.
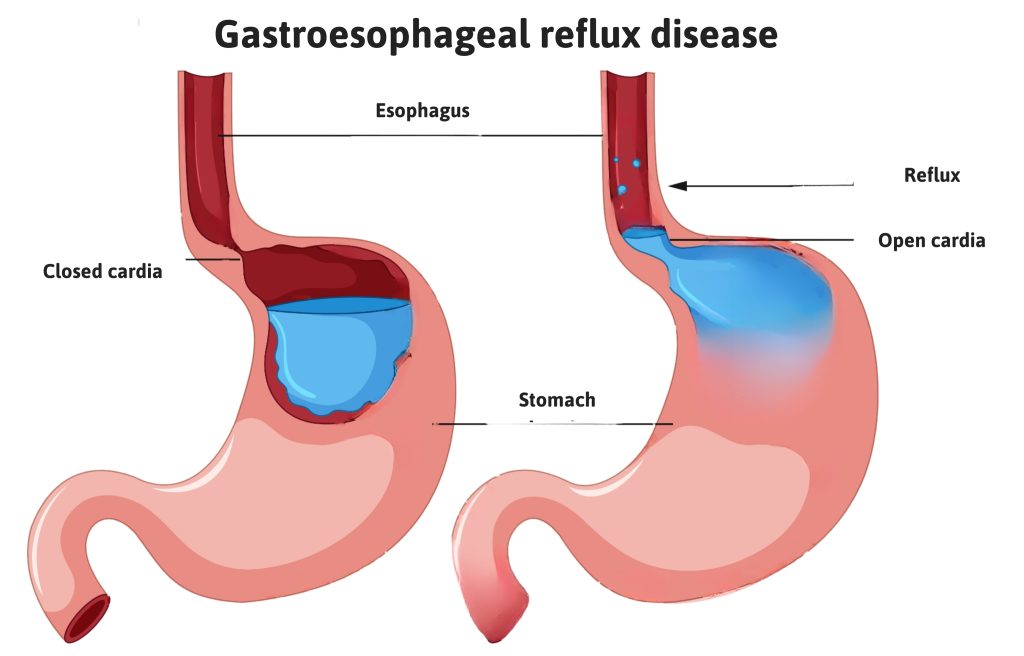
According to Dr Ngo Van Huy, treatment for acid reflux has traditionally relied on acid-suppressing medications or Nissen surgery. However, these approaches have several limitations. Medication typically offers only temporary relief, while Nissen surgery is complex, can be painful, requires several days in hospital, and involves a lengthy recovery period.
The technique of endoscopic cardiac sphincter tightening involves the use of a specialized band to apply appropriate pressure at the cardiac sphincter. This process stimulates the formation of natural scar tissue, which helps the sphincter close more effectively and prevents stomach acid from flowing back into the oesophagus.
For patients with Barrett’s oesophagus, like Mr P., the Argon Plasma technique will be applied alongside treatment. “The mechanism of Argon plasma is to use high-frequency electrical energy to convert Argon gas into plasma form to destroy the pathological Barrett cells. The digestive endoscopist can adjust the current intensity to control the penetration of the Argon Plasma flow, selectively destroying the diseased tissue while protecting the adjacent healthy tissue, ensuring accuracy and safety for the procedure,” Dr Huy explained.
Mr P.’s procedure was performed by Dr Ngo Van Huy and lasted about 60 minutes. The cardiac sphincter tightened first, followed by Argon plasma treatment applied to the Barrett’s areas in the oesophagus the next day. Mr P. was discharged later that same day.
In the days that followed, Mr P.’s health improved significantly, and the chest discomfort that had troubled him for years disappeared. “Now, I truly feel optimistic and comfortable. It’s been so long since I’ve felt this way. I am deeply grateful to the team of doctors and nurses at FV Hospital. They treated and cared for me with great dedication and attention,” Mr P. shared emotionally.

Gastro-oesophageal Reflux: Many Hidden Risks
According to Dr Ngo Van Huy, GERD was once more prevalent in Western countries. However, in recent years, the incidence has increased rapidly in Vietnam, now affecting nearly 20% of the population. Furthermore, about 1.3% of Asian patients with GERD go on to develop Barrett’s oesophagus.
Reflux can be caused by a variety of factors, with unhealthy eating habits, excessive consumption of alcohol and coffee, spicy foods, and late-night eating among the primary risks. Obesity, increased abdominal pressure, and prolonged stress also contribute to the likelihood of stomach acid flowing back up into the oesophagus.
GERD not only affects quality of life but also poses several risks. “Many people mistakenly think that reflux is just heartburn, but in fact, it is a chronic digestive disease that can lead to oesophageal ulcers, oesophageal strictures, and most dangerously, Barrett’s oesophagus, a pre-cancerous condition,” Dr Huy explains.
Dr Huy advises that anyone experiencing prolonged heartburn, throat discomfort, or difficulty swallowing after meals for more than a few weeks should seek medical attention promptly. This allows for an accurate diagnosis and appropriate treatment, helping prevent the disease from progressing to a dangerous stage.
Dr Huy mentioned that over 100 patients at FV Hospital have been successfully treated using the endoscopic fundoplication technique. The outcomes have been very positive, with a significant reduction in reflux symptoms and a near-zero complication rate. This is considered an optimal solution for patients who have not responded to medication, those with Barrett’s oesophagus, or those with severe complications such as oesophageal ulcers. It is also suitable for individuals who are unwilling or unable to undergo surgery due to health reasons.
To learn more about these techniques, please contact the Gastroenterology & Hepatology Department at FV Hospital on (028) 54 11 33 33.

 Vi
Vi 











