Work in the Intensive Care Unit (ICU) at FV Hospital is a blend contradiction. Here, there is the presence of life and death, joys and sorrows, where individuals silently holding on to each life amidst the busy work.
Every day brings hundreds of concerns.
On the monitor screens at the ICU today, almost every room has patients under care. Some are having wounds cleaned and bandages changed; some are undergoing maintenance of catheters, endotracheal tubes, infection control intervention; others are preparing for movement and respiration sessions with physical therapists. In another room, a nurse is assisting a nutrition specialist in evaluating the patient’s condition. Not confined to their own group tasks, ICU nurses must connect with various specialists to create a comprehensive care programme for their patients.

ICU nurses can monitor the condition of all patients from the central screens.
Ms Dam Thi Hoa (ICU nurse), often called Soeur Hoa, is completing the nursing care record recording for the morning shift. Every aspect of care progress is detailed, to report any abnormal signs to the doctors. All notes are typically written in English – the language encouraged in medical records at FV Hospital.
The working hours in the ICU are divided into three shifts, and the busiest time is during the shift handover. It is almost 2 p.m., and the handover still shows no sign of ending, even though it has been going for 30 minutes. Nurses in pairs rotate around a stack of patient records. Taking notes, asking questions, then jotting down, repeating the process to ensure the next shift receives the correct treatment plan. People grab lunch right after the handover. This “daily exchange” seems endless.

Even small details must be clearly communicated to the next shift.
Mr Do Chi Tam (ICU Head Nurse) laughs, saying, “During break time, everyone is pro-active, but sometimes we have to remind them to rest.” Young nurses can get absorbed in their work, forgetting themselves, as a couple of minutes of neglect might impact a patient’s ICU experience. Like sentinels, nurses inform each other when they need to step out, have a meal, or take a break. It’s not only to ensure safe treatment but also to make the nurse feel more at ease.
During mealtime, which is always uncertain in the ICU, stories revolve around life events, intertwined with the condition of their patients or the transferred cases from other wards. Health matters sometimes outweigh family concerns. Ms Chau puts down her chopsticks halfway through her meal, washes her hands, put her mask on, and returns to assist a patient. On the other side of the table, Ms Phung says she wants to leave early today to take care of her sick child at home. “I thought of taking the day off this morning, but Mr Tâm reported that the patient needs a lot of support,” she explains. She takes advantage of lunchtime – also a break time – to review tasks that still need to be completed.

Mealtime often turns into a time for task exchange in the ICU.
Outside, the steady rhythm of vital sign monitors, the hiss of air pumping from the ventilators, and the on-going exchange of voices blend together. That regular “bustle” signal those temporarily “resting between half’s” that everything is well under control, and they can take a moment to finish their meal. However, there are still many un-eaten portions of rice on the table, many unfinished dishes, and often meals left cold until late afternoon.
Contemplating each life
Mr Tam shares that an ICU nurse must be adept not only at distinguishing sounds within the treatment area but also understanding what those sounds convey and whether there is anything unusual. However, the mantra of “eyes, ears, and hands always busy” does not necessarily create immense pressure here. In the ICU, there are many invisible psychological pressures.
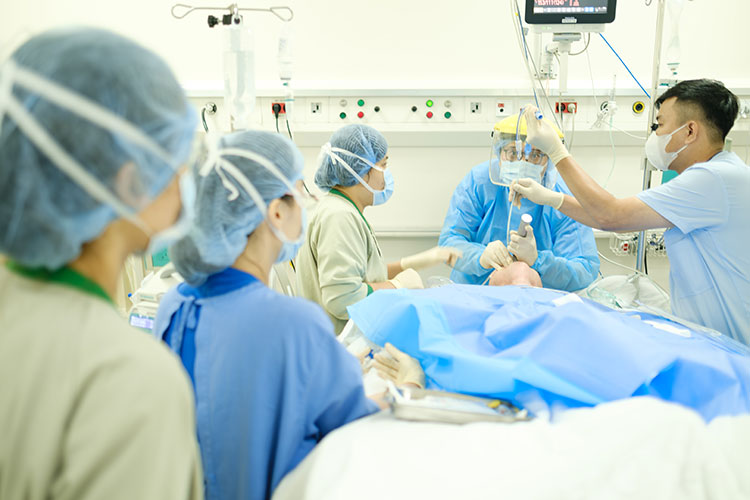
This morning, the ICU had a patient with postpartum complication, having undergone surgery four times in one month in Cambodia to address uncontrolled bleeding she was finally transferred to FV. Every 30-60 minutes, a nurse in full personal protective equipment (PPE) will enter the isolation room to care for this patient. “There are cases that require more manpower, equipment, and time to ensure patient safety,” Mr Tam says.
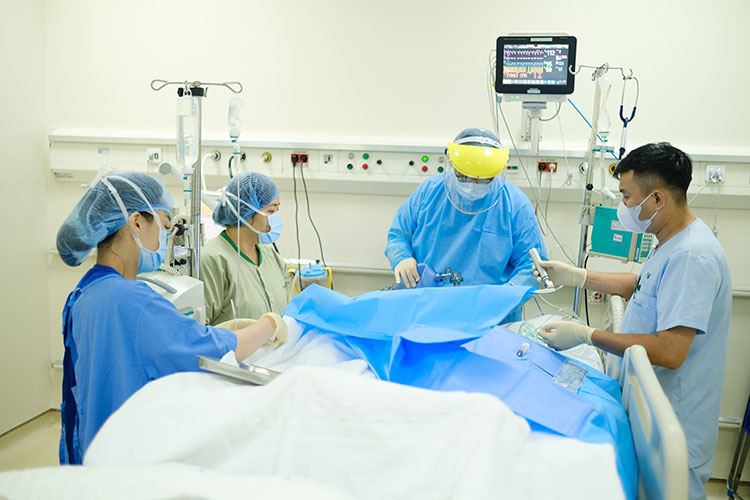
Continuous exposure to critical cases creates significant mental pressure for doctors and nurses in the ICU.
All members of the care team hope this new mother responds to treatment, and the bleeding can be controlled today. Not just out of empathy for a young mother or concern for the hospital’s treatment effectiveness, but prolonging even a day of treatment for this mother will impose a significant economic burden on the family. This adds to the sense of responsibility and psychological burden felt by the nurses.
FV ICU is located on the second floor, and in 20 years of working here, both Soeur Hoa and Mr Tam cannot recall how many patients were transferred out to the regular wards (floors 4, 5, 6) or sometimes the mortuary on the ground floor. However, they are both certain that cases that return home with life represent a much higher percentage than those with a more regretful outcome. “Nevertheless, informing family members to mentally prepare for the impending negative outcome is not an easy task, especially for young nurses,” Soeur Hoa says.
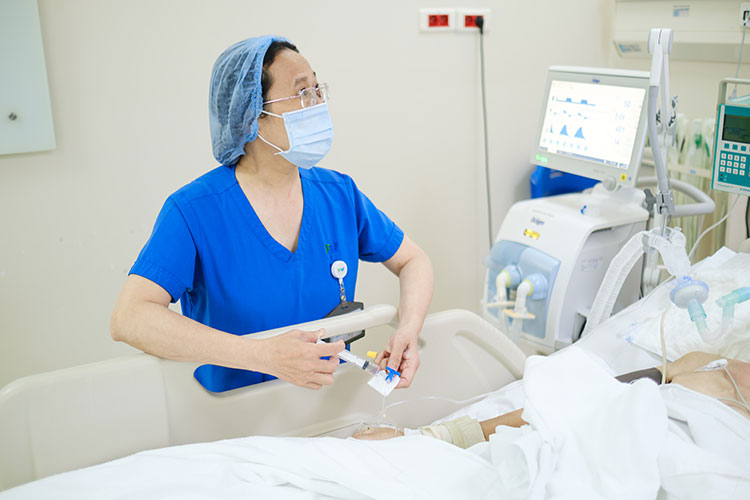
Balancing professional and personal life is essential for enduring the stress in the Intensive Care Unit.
Behind Soeur Hoa, Mr Ha Gia Phong (Ward Charging Secretary – ICU) just finished a call explaining treatment costs to a family member. Phong says, “Initially, when announcing the treatment costs for severe cases or deaths, I was very anxious. But overall, families react reasonably.” Phong explains that, in the leading up, doctors and nurses shared not only detailed information about the treatment but also show empathy and provided psychological support to the families. “They understand that we have done our best, so my part is more bearable. Because the pressure was already intense for doctors and nurses in the previous stage,” Phong adds.
The hurried meals, the bustling pace, or the invisible pressures are sometimes requirements of those who love the busy atmosphere. However, in the ICU, the life of an individual is not only represented by numbers or statistics on devices but is also present in the hustle and bustle atmosphere at the hospital. Those are the truly precious hurried moments.

 Vi
Vi 










