FV Hospital successfully treated two patients with rare gynaecological emergencies – torsion of a pedunculated uterine fibroid and adnexal torsion in pregnancy – through prompt multidisciplinary collaboration. Both patients initially reported common symptoms such as abdominal pain and nausea.
Suspected digestive disorder turns out to be a rare gynaecological complication
T.T., a 29-year-old woman from Ho Chi Minh City, was admitted with lower abdominal pain and diarrhoea, initially suggestive of a gastrointestinal issue. Initial investigations found no abnormalities other than a known uterine fibroid (leiomyoma), and she was discharged after treatment.
Within 48 hours, her pain worsened and inflammatory markers increased. On her return, a multidisciplinary team conducted a thorough re-evaluation. Repeat imaging showed a large fibroid with reduced blood flow. Based on clinical and laboratory findings, the team diagnosed torsion of a pedunculated subserosal uterine fibroid, a rare complication seen in fewer than 0.25% of subserosal fibroid cases.
She was immediately taken to the operating theatre for emergency laparoscopic surgery. The procedure revealed complete axial torsion of the large pedunculated fibroid, causing total vascular occlusion. As Dr Vo Trieu Dat, MSc, explained: “Delaying the surgical intervention would have carried a substantial risk of irreversible ischaemic injury to the adjacent tissue and organs, leading to potentially life-threatening sequelae such as necrosis, septicaemia, and peritonitis.”
Due to prompt and accurate diagnosis, the laparoscopic procedure was completed without complications, and the patient was discharged two days later.
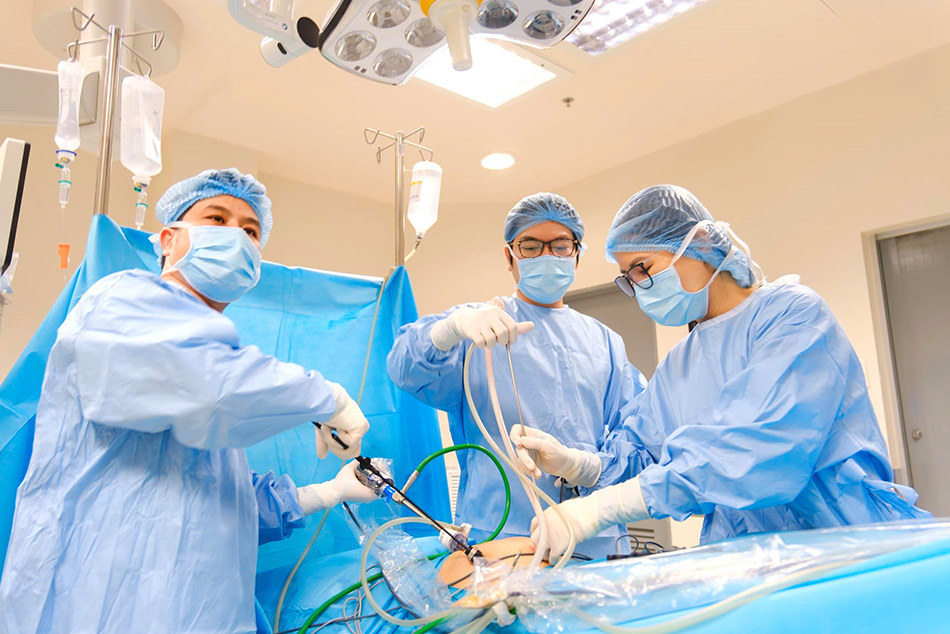
Dr Vo Trieu Dat (centre) and the laparoscopic surgical team during the procedure. (Photo: FV)
Emergency management of adnexal torsion in a pregnant patient
A 30-year-old woman, identified as X.A., presented to FV Hospital with mild pain in the right iliac fossa. Within 24 hours, her pain intensified and was accompanied by nausea and vomiting. Ultrasound revealed significant enlargement of the right ovary, nearly double its normal size. Dr Vo Trieu Dat, MSc, promptly organised a multidisciplinary consultation with surgical and diagnostic imaging specialists. The team diagnosed adnexal torsion at 5-6 weeks’ gestation.
Dr Vo Trieu Dat, MSc, said: “Adnexal torsion during pregnancy is exceedingly rare, with an incidence rate of approximately 1.6 per 10,000 pregnancies.” Initial symptoms often resemble more common obstetric and gastrointestinal conditions, such as threatened miscarriage, pre-term labour, and gastritis, which increases the risk of misdiagnosis. About 57% of adnexal torsion cases present with intermittent pain, making diagnosis more challenging. If surgical detorsion is performed within the first 24 hours, ovarian conservation rates can reach 84%. Delayed diagnosis may prevent timely intervention, leading to serious consequences for both mother and foetus. These include ovarian necrosis, long-term endocrine and reproductive issues for the mother, and increased risks of miscarriage, pre-term labour, or intra-uterine foetal demise due to ischaemia.
The patient underwent emergency laparoscopic surgery. After detorsion, the ovary gradually regained its blood supply, indicating timely intervention. She was discharged 2 days later, and her pregnancy continued to progress normally.
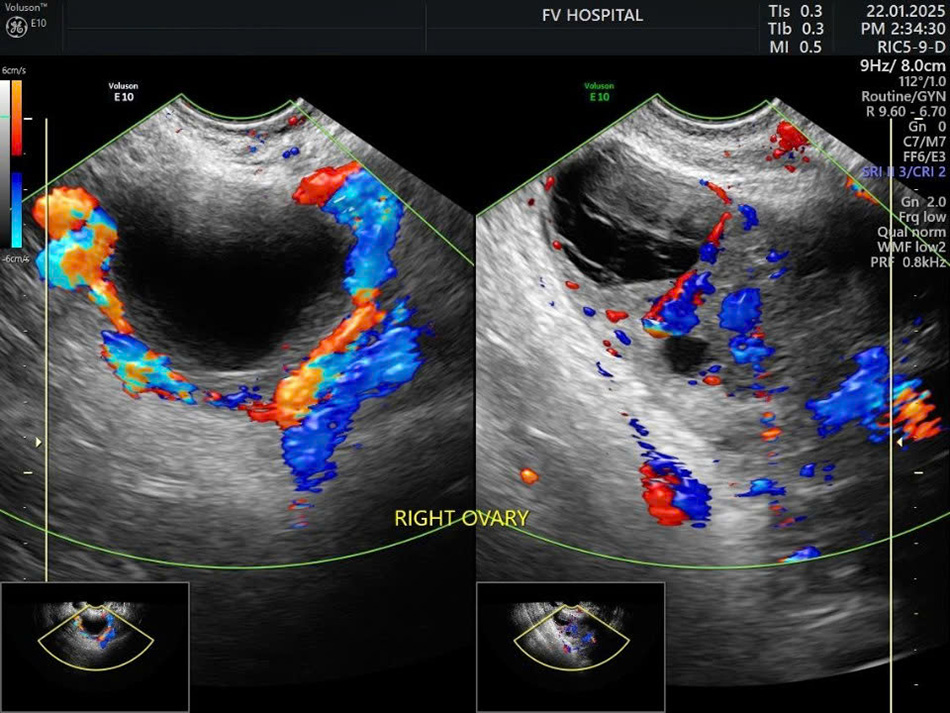
One week follow-up ultrasound: The image on the left displays the torted ovary, while the image on the right demonstrates normal reperfusion of the ovary post-surgery.
Multidisciplinary collaboration: a decisive factor in managing complex cases
Dr Vo Trieu Dat, MSc – FV Thomson Maternity observed that both cases presented atypically, closely resembling more common conditions and resulting in significant diagnostic uncertainty.
“The main challenge was not the surgery itself, but making the correct diagnosis. Assessing clinical data in isolation can easily lead to errors. Multidisciplinary collaboration was essential, enabling us to synthesise the full clinical picture and make timely treatment decisions,” he said.
At FV Hospital, a multidisciplinary approach is now standard practice for managing complex cases. This strategy significantly improves diagnostic accuracy and optimises patient outcomes.
Insights from these cases were recently shared at the Continuing Medical Education (CME) conference “Clinical challenges in the management of gynaecological pathologies”, hosted by the hospital on March 21, 2026. The event drew over 700 clinicians and specialists. In addition to updating clinical knowledge, the conference offered a valuable forum for sharing expertise in managing rare and diagnostically challenging cases in daily practice.

Attendees at the CME conference “Clinical challenges in the management of gynaecological pathologies”.
The strong interest from the medical community underscores the growing need for integrated treatment approaches and reaffirms FV Hospital’s leadership in obstetrics and gynaecology in southern Vietnam.
The introduction of the da Vinci Xi robotic surgical system has further strengthened the hospital’s ability to manage complex cases. This technology enables surgeons to operate with greater precision and dexterity, reducing blood loss and speeding patient recovery.

 Vi
Vi 












